
Contactless vital signs monitoring
The COVID-19 pandemic has accelerated methods to facilitate contactless evaluation of patients in hospital settings. By minimizing in-person contact with individuals who may have COVID-19, healthcare workers can prevent disease transmission and conserve personal protective equipment. Obtaining vital signs is a ubiquitous task that is commonly done in person by healthcare workers. To eliminate the need for in-person contact for vital sign measurement in the hospital setting, we developed Dr. Spot, a mobile quadruped robotic system. The system includes IR and RGB cameras for vital sign monitoring and a tablet computer for face-to-face medical interviewing. Dr. Spot is teleoperated by trained clinical staff to simultaneously measure the skin temperature, respiratory rate, and heart rate while maintaining social distancing from patients and without removing their mask. To enable accurate, contactless measurements on a mobile system without a static black body as reference, we propose novel methods for skin temperature compensation and respiratory rate measurement at various distances between the subject and the cameras, up to 5 m. Without compensation, the skin temperature MAE is 1.3°C. Using the proposed compensation method, the skin temperature MAE is reduced to 0.3°C. The respiratory rate method can provide continuous monitoring with a MAE of 1.6 BPM in 30 s or rapid screening with a MAE of 2.1 BPM in 10 s. For the heart rate estimation, our system is able to achieve a MAE less than 8 BPM in 10 s measured in arbitrary indoor light conditions at any distance below 2 m.

-
H.-W. Huang*, J. Chen*, P.R. Peter*, C. Ehmke*, P. Rupp, F. Z. Dadabhoy, A. Feng, A. J. Thomas, M. da Silva, M. Raibert, E. W. Boyer, G. Traverso, “Mobile robotic platform for contactless vital signs monitoring,” Cyborg and Bionic Systems, 9780497, 2022 (Selected as the journal cover)
-
P. R. Chai, F. Z. Dadabhoy, H.-W. Huang, J. N. Chu, A. Feng, H. Le, M. da Silva, M. Raibert, C. Hur, E. W. Boyer, G. Traverso, “Assessment of the Acceptability and Feasibility of Using Mobile Robotic Systems for Patient Evaluation,” JAMA network open, 2021
-
P. R. Chai, P. Rupp, H.-W. Huang, J. Chen, C. Vaz, A. Sinha, C. Ehmke, A. Thomas, F. Z. Dadabohy, J. Y. Liang, A. A. Landman, G. Player, K. Slattery, G. Traverso, ”The acceptance of a computer vision facilitated protocol to measure adherence to face masks: a single site, observational cohort study among hospital staff,” BMJ Open,12 (12), e062707, 2022
Cost-effective Mobile Solution for Autonomous and
Continuous Vital Signs Monitoring
Despite promising performance, the use of static camera setups requires subjects to remain static inside a field of view (FoV) for a prespecified duration. Due to inconsistent ambient environmental conditions, the transit of individuals through the FoV, and the time it may take to triage individuals, the widespread adoption of static camera systems to continuously monitor vital signs has had suboptimal uptake. Robotic systems enable autonomous and continuous monitoring, but these require expensive cameras, computers, and robotic platforms, limiting widespread deployment. In response, we propose a cost-effective and scalable robotic solution consisting of two parts: 1) a suite of commercial, off-the-shelf wireless cameras for capturing photoplethysmography (PPG) on ambulatory subjects linked to a single computer that supervises the cameras to compute the vital signs of subjects; 2) a hybrid centralized/decentralized wireless machine vision protocol for enabling enable real-time streaming of high-quality PPG from multiple cameras simultaneously. Our results demonstrate that the proposed cost-effective wireless camera achieves equivalent remote-PPG accuracy to its costly, USB3 counterparts (5.0 BMP vs. 4.7 BPM) by means of the hybrid camera protocol which boosts the overall frame rate to 17 FPS. In contrast, using the standard method that captures the PPG with the same spatial resolution can only achieve 1 FPS. We also show that the proposed hybrid protocol--which partially offloads PPG computation and region of interest (ROI) tracking from the PC to the camera-enables simultaneous monitoring of five subjects while maintaining the same frame rate and rPPG accuracy using just one computer.



-
H.-W. Huang, P. Rupp, J. Chen, I. Ballinger, P. R. Chai, G. Traverso, “Cost-Effective Solution of Remote Photoplethysmography Capable of Real-Time, Multi-Subject Monitoring with Social Distancing,” IEEE Sensors, Dallas, USA, 2022
-
J. Chen*, H.-W. Huang*, P. Rupp, A. Sinha, C. Ehmke, G. C. Traverso, ”Closed-Loop Region of Interest Enabling High Spatial and Temporal Resolution via Wireless Camera,” IEEE Access,*equal contribution, 2021
Autoclavable mask
N95 filtering facepiece respirators (FFR) and surgical masks are essential in reducing airborne disease transmission, particularly during the COVID-19 pandemic. However, currently available FFR’s and masks have major limitations, including masking facial features, waste, and integrity after decontamination. In a multi-institutional trial, we evaluated a transparent, elastomeric, adaptable, long-lasting (TEAL) respirator to evaluate success of qualitative fit test with user experience and biometric evaluation of temperature, respiratory rate, and fit of respirator using a novel sensor. There was a 100% successful fit test among participants, with feedback demonstrating excellent or good fit (90% of participants), breathability (77.5%), and filter exchange (95%). Biometric testing demonstrated significant differences between exhalation and inhalation pressures among a poorly fitting respirator, well-fitting respirator, and the occlusion of one filter of the respirator. We have designed and evaluated a transparent elastomeric respirator and a novel biometric feedback system that could be implemented in the hospital setting.
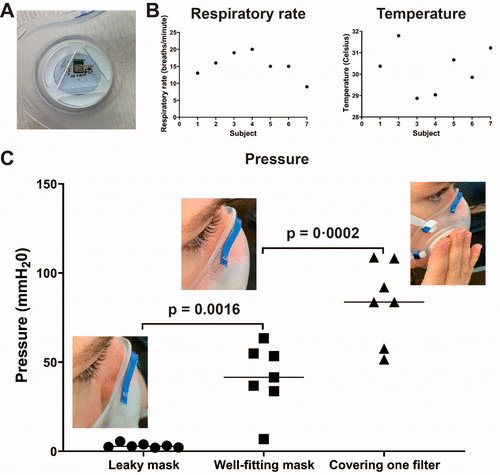
Clinical evaluation of customized respirator sensor for biometrics. (A) Active sensors on printed circuit board within the respirator. (B) Respiratory rate and exhalation breath temperature (n = 7) and (C) pressure differences in respirator between exhalation and inhalation in setting of leaky respirator, well-fitting respirator, and covering one filter with hand (n = 7).
-
A. J. Wentworth, J. D. Byrne, S. Orguc, J. Sands, S. Maji, C. Tov, S. Babaee, H.-W. Huang, H. Boyce, P. R. Chai, S. Min, C. Li, J. N. Chu, A. Som, S. L. Becker, M. Gala, A. Chandraskasan, G. Traverso, “Multi-Institutional Prospective Evaluation of the Transparent, Elastomeric, Adaptable, Long-lasting (TEAL) Respirator,” ACS Pharmacol. Transl. Sci., 2020
-
J. D. Byrne*, A. J. Wentworth*, P. R. Chai*, H.-W. Huang*, S. Babaee, C. Li, S. L. Becker, C. Tov, S. Min, G. Traverso, “Injection Molded Autoclavable, Scalable, Conformable (iMACS) system for Aerosol-based Protection,” BMJ Open, vol. 10, no. 7, pp. e039120, 2020 *equal contribution